We have all heard of retinal detachment at some point, whether on television, in a magazine or newspaper, in a health blog, or from someone we know, but do we really know what retinal detachment is?
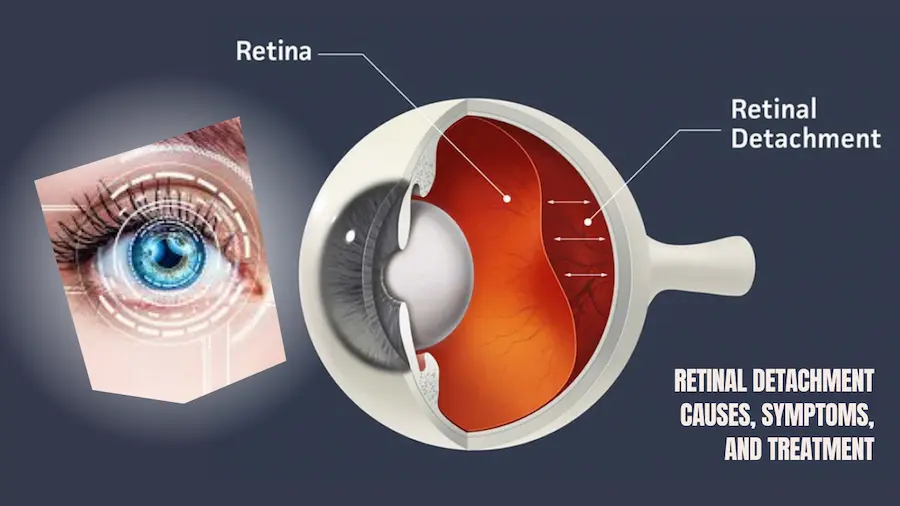
God Service Eye Clinic says retinal detachment is a serious eye condition that occurs when the retina, the thin and light-sensitive tissue at the back of the eye, detaches or separates from its normal position. The retina plays a crucial role in vision by capturing light and sending signals to the brain for image interpretation.
Let’s learn about retinal detachment, its causes, symptoms, and treatments in this blog.
What is retinal detachment?
The retina is the innermost layer of the back half of the eye. It is responsible for receiving light and sending images to the brain for them to be processed. Retinal detachment is the separation of this layer from its supporting anatomical position.
It is caused by the separation of the neurosensory retina (inner layer of the retina) from the adjacent layer, called the choroid. When these two layers separate, they create a virtual space that begins to collect fluid.
A retinal detachment is an ophthalmological emergency that can happen at any age and without any history of the disease, so it is vitally important to have regular check-ups. According to studies, retinal detachments can affect one in 10,000 people a year.
Causes of retinal detachment
It usually occurs in middle to elderly people, affecting more men than women and whites more than African-Americans. Those who have myopia, family history, or previous retinal detachments are more at risk of suffering from it.
One of the main causes of retinal detachments is the existence of one or more tears in the retina, which can also occur due to eye trauma or after surgery such as cataract surgery. Other causes could be tumors in the choroid, myopic macular holes (people with high myopia), diabetic retinopathy, or severe eye inflammation.
What are the symptoms of retinal detachment?
In our ophthalmology offices, floating spots and light flashes are quite common and frequent, but they are not always indicators of a retinal tear or detachment. However, they are reason enough to go immediately to the ophthalmologist and rule out any serious ocular involvement. The symptoms of retinal detachment are:
- A sudden increase in the size or number of floaters, small greyish or dark spots, called floaters.
- The sudden appearance of light flashes, like lightning bolts, is called photopsia.
- The appearance of a grey curtain or a black curtain in the form of a veil that affects our visual field.
- A sudden decrease in visual acuity.
Retinal detachment treatment
Most people with retinal detachment need to be treated immediately or within a short period of time after diagnosis. The treatments seek to fix the retina back to its original position by creating a scar that seals that area that was detached. With this we avoid the passage of fluid through the tear, preventing the retina from detaching again. There are several types of treatments:
- Laser photocoagulation: therapeutic burns are created in a detached area of the retina. These laser areas end up healing and thus sealing the retina, making it possible for the vitreous humor not to pass under the retina and for the detachment to be reversed.
- Vitrectomy: Vitrectomy is a surgical procedure where the vitreous humor, which pulls on the retina, is usually replaced by a bubble of gas, liquid, air, or silicone oil to help hold the retina in place.
- Cryotherapy: With a cryoprobe, the part surrounding the torn area is frozen, thus forming a protective scar, similar to the laser photocoagulation technique.
- Pneumatic retinopexy: This technique consists of introducing a gas bubble into the eye, thus creating pressure on the detached area of the retina, helping to heal and avoiding its extension.
- Scleral closure or scleral ring: It is a surgical process where a ring or band is placed surrounding the external part of the wall of the eye, the sclera, thus creating external pressure on the eyeball that does not allow the spread of retinal detachment.
Depending on the type of retinal detachment and the surgical treatment chosen, your ophthalmologist will ask you to keep your head in a certain position during the postoperative period, to facilitate the correct repositioning of your retina. The specialist will determine the time of absolute rest since practicing sports activities or lifting heavy objects must be limited to guarantee the success of the surgical intervention.
How to prevent it?
The prognosis after a retinal detachment depends on the location and extent of the detachment, as well as prompt treatment. The visual prognosis can be excellent if the macula has not suffered any damage. Sometimes, successful surgical repair of the retina does not ensure full recovery of visual acuity. To prevent a retinal detachment it is very important to go to your ophthalmologist at least once a year to do a fundus examination. If we suffer from any symptoms of retinal detachment of those previously exposed, go to the ophthalmologist as soon as possible.







Leave a Reply